IED is more likely to be found in some epilepsy syndromes or seizure types.
Children are more likely to than older subjects. The incidence increases substantially to 10–30% in cerebral pathologies such as tumour, prior head injury, cranial surgery, or congenital brain injury 3 particular caution is necessary when evaluating the significance of IED in such cases, and especially when the clinical history offers little support for a diagnosis of epilepsy.Ī number of factors influence whether patients with epilepsy will show IED in the EEG. 2 A slightly higher incidence of 2–4% is found in healthy children and in non-epileptic patients referred to hospital EEG clinics. How often and in which circumstances do non-epileptic subjects show IED in the EEG? In healthy adults with no declared history of seizures, the incidence of epileptiform discharge in routine EEG was 0.5%. Misinterpretation of such non-epileptogenic phenomena, or overinterpretation of non-specific EEG abnormalities and spiky/paroxysmal variants of normal cerebral rhythms, are a common reason for over-diagnosis of epilepsy. Spikey or rhythmic phenomena such as 14 and 6 Hz spikes, phantom spike and wave, rhythmic mid temporal theta (θ), psychomotor variant and subclinical rhythmic epileptiform discharge in adults (SREDA), have low or zero predictive value for epilepsy. Of children with centro-temporal or rolandic EEG discharges, only about 40% have clinically expressed seizures. Some types of epileptiform phenomena-3 per second spike wave discharge, hypsarrhythmia, and generalised photoparoxysmal response-are strongly correlated with clinical epilepsy, whereas focal sharp waves in centro-temporal or occipital regions have moderate association with clinically active epilepsy. Abnormalities of background cerebral rhythms, focal slow activity or regional attenuation are much less specific than epileptiform activity, although they can indicate localised structural pathology underlying the seizure disorder, or diffuse cortical dysfunction as in symptomatic generalised epilepsies.
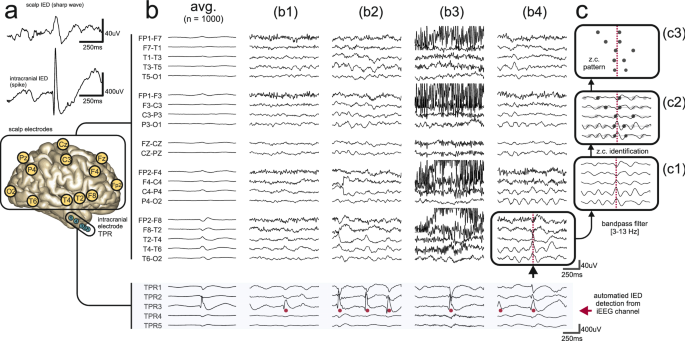
Secondly, correlation between different EEG patterns and epilepsy varies, and only IED are associated with seizure disorders at a sufficiently high rate to be of clinical use. These wide ranges can be explained partly by diverse case selection and differences in clinical requirements for diagnosis of epilepsy in population studies of EEG specificity and sensitivity. Specificity is better, but again variable at 78–98%. EEG has relatively low sensitivity in epilepsy, ranging between 25–56%. SPECIFICITY AND SENSITIVITY OF ROUTINE EEGĮpileptiform activity is specific, but not sensitive, for diagnosis of epilepsy as the cause of a transient loss of consciousness or other paroxysmal event that is clinically likely to be epilepsy. Temporal sampling is also limited, and the relatively short duration of routine interictal EEG recording is one reason why patients with epilepsy may not show interictal epileptiform discharge (IED) in the first EEG study. Spatial sampling in routine scalp EEG is incomplete, as significant amounts of cortex, particularly in basal and mesial areas of the hemispheres, are not covered by standard electrode placement. Cortical generators of the many normal and abnormal cortical activities recorded in the EEG are still largely unknown. Propagation of electrical activity along physiological pathways or through volume conduction in extracellular spaces may give a misleading impression as to location of the source of the electrical activity. Quite large areas of cortex-in the order of a few square centimetres-have to be activated synchronously to generate enough potential for changes to be registered at electrodes placed on the scalp. Electrical activity recorded by electrodes placed on the scalp or surface of the brain mostly reflects summation of excitatory and inhibitory postsynaptic potentials in apical dendrites of pyramidal neurons in the more superficial layers of the cortex. However, the EEG has a number of limitations. EEG continues to play a central role in diagnosis and management of patients with seizure disorders-in conjunction with the now remarkable variety of other diagnostic techniques developed over the last 30 or so years-because it is a convenient and relatively inexpensive way to demonstrate the physiological manifestations of abnormal cortical excitability that underlie epilepsy. Its potential applications in epilepsy rapidly became clear, when Gibbs and colleagues in Boston demonstrated 3 per second spike wave discharge in what was then termed petit mal epilepsy. The human electroencephalogram (EEG) was discovered by the German psychiatrist, Hans Berger, in 1929.
